Blog
Clinical evidence insights, methodology deep-dives, and the latest in clinical decision support from the Ailva team.

Sepsis Management: From Early Recognition to Evidence-Based Resuscitation
The Surviving Sepsis Campaign 2024 guidelines refined the approach to sepsis resuscitation, antibiotic timing, and vasopressor selection. This review covers the current evidence for hour-1 bundle compliance, fluid strategy, and organ support.

GOLD 2026 COPD Guidelines: Triple Therapy, Biologics, and Exacerbation Prevention
The 2026 GOLD report updates the COPD management framework with revised ABCD grouping, expanded triple therapy recommendations, and emerging biologic therapies for eosinophilic COPD. A practical guide for pulmonologists and primary care.

Antibiotic Stewardship 2026: Resistance Trends and Empiric Therapy Updates
Antimicrobial resistance continues to accelerate globally. This review covers updated empiric therapy recommendations, de-escalation strategies, and the role of rapid diagnostics in optimizing antibiotic prescribing for common infectious syndromes.
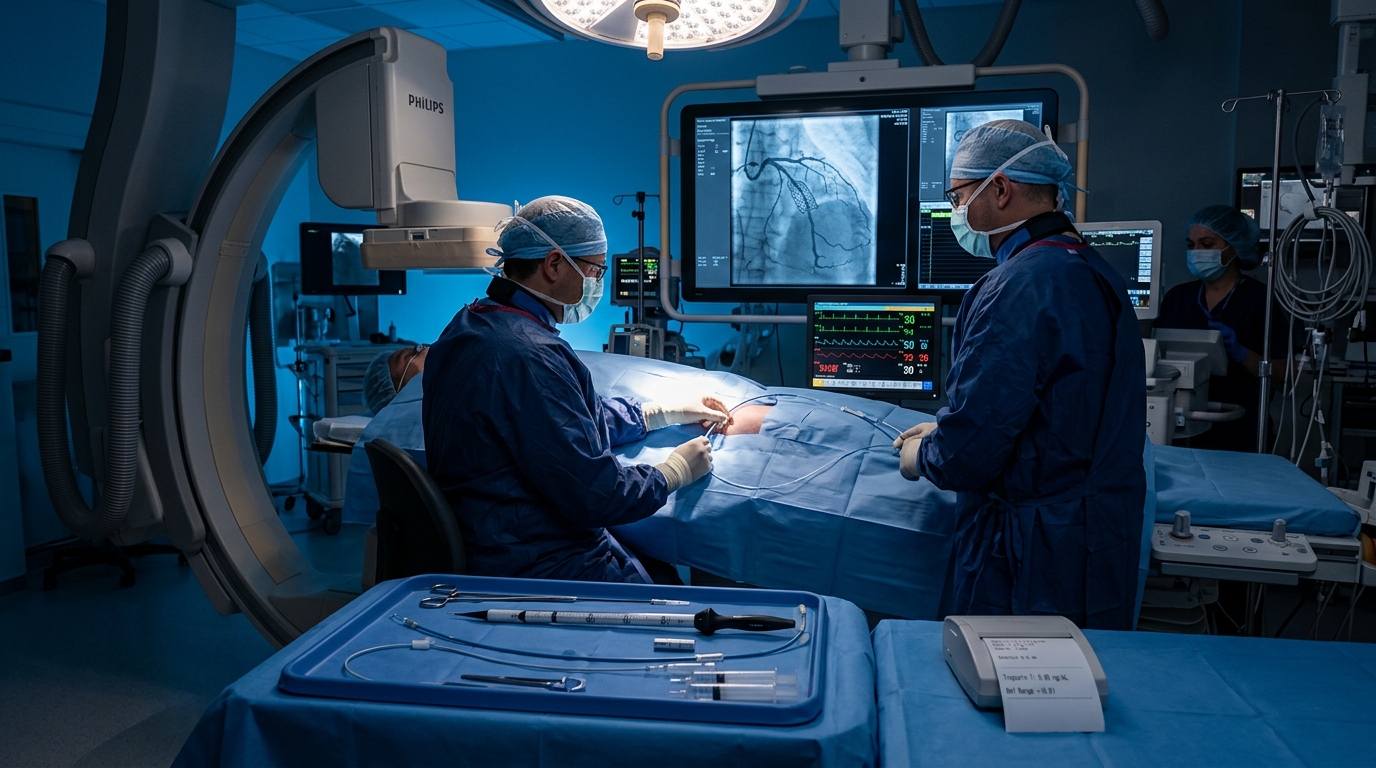
Acute Coronary Syndrome: STEMI and NSTEMI Management Updates for 2026
Recent trial data from FIRE, MULTISTARS AMI, and TOMAHAWK have refined revascularization strategy, timing, and antiplatelet selection in ACS. This article reviews the current evidence for complete revascularization, de-escalation antiplatelet therapy, and risk-stratified NSTEMI management.
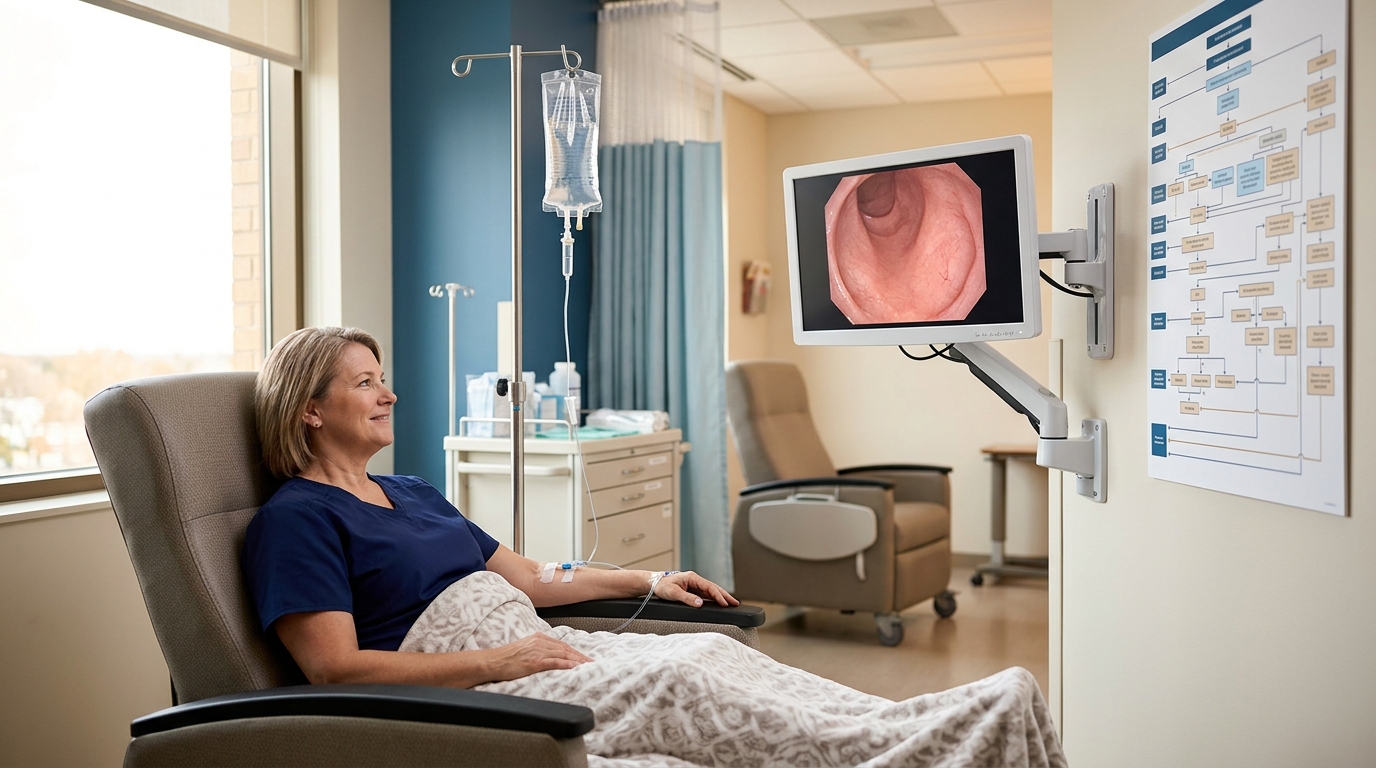
IBD Management: Vedolizumab, Ustekinumab, and JAK Inhibitors in UC and Crohn Disease
The IBD therapeutic landscape has expanded beyond TNF inhibitors to include gut-selective integrins, IL-12/23 blockade, and JAK inhibitors. This review compares positioning, efficacy endpoints, and safety profiles of vedolizumab, ustekinumab, tofacitinib, and upadacitinib in ulcerative colitis and Crohn disease.

Osteoporosis Pharmacotherapy: Romosozumab, Denosumab, and Sequential Therapy Strategy
The osteoporosis treatment paradigm has shifted from bisphosphonate monotherapy to anabolic-first sequential strategies. This review covers romosozumab efficacy data, denosumab rebound fracture risk, and evidence-based sequencing for high-risk patients.
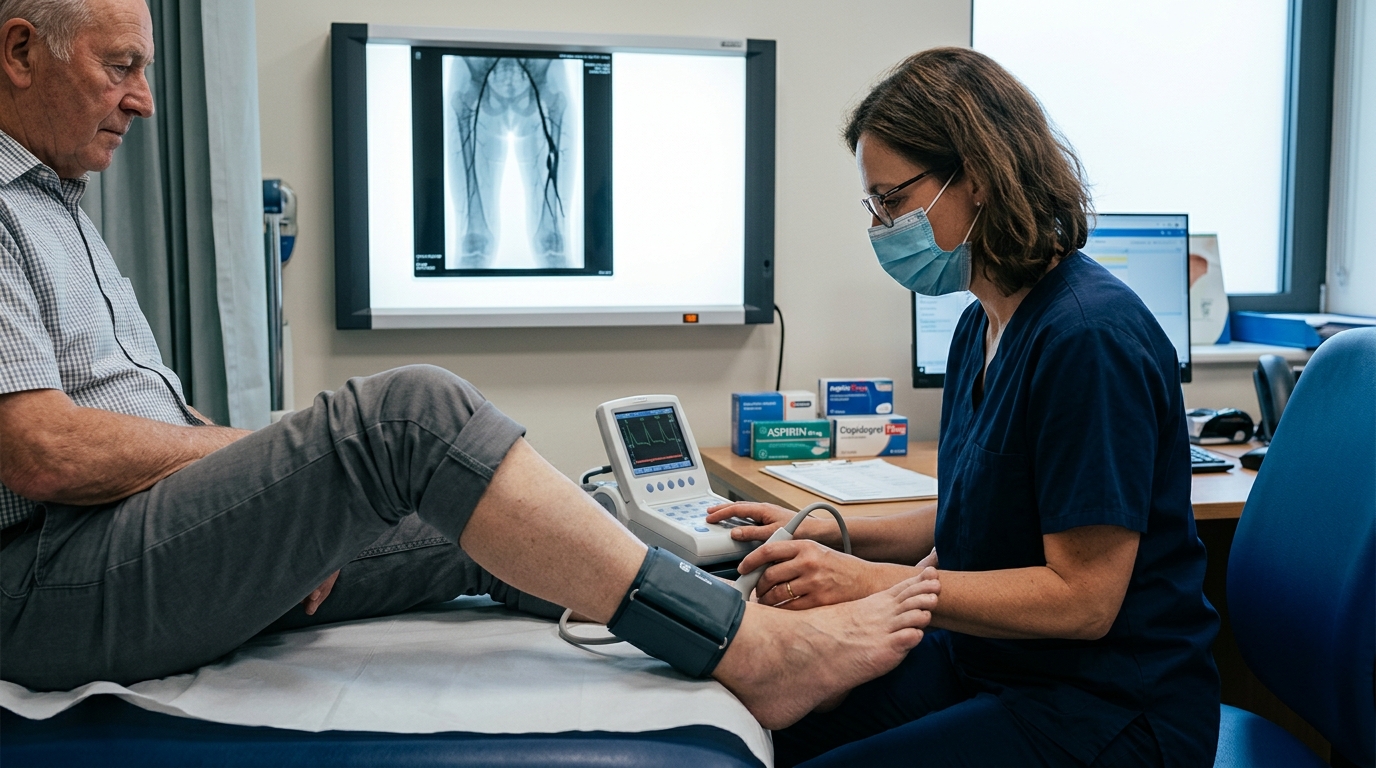
Peripheral Artery Disease: Revascularization vs Medical Therapy and VOYAGER PAD Data
The BEST-CLI and VOYAGER PAD trials have refined PAD management, clarifying when revascularization improves outcomes and how to optimize antithrombotic therapy post-intervention. This review covers the evidence for medical management versus revascularization, CLTI staging, and dual-pathway inhibition.
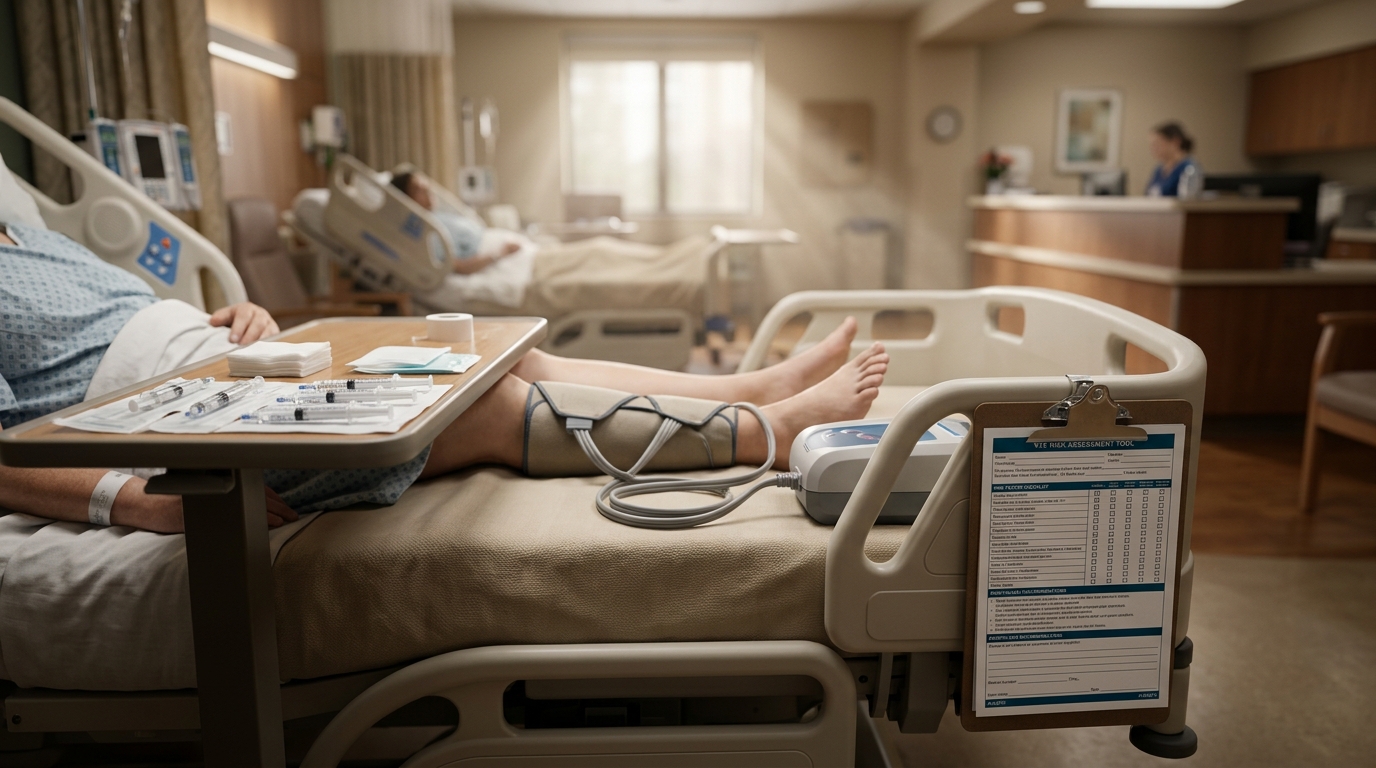
Venous Thromboembolism Prevention: Post-Surgical and Medical Prophylaxis Strategies
VTE remains a leading cause of preventable hospital death, with 60% of VTE events associated with recent hospitalization. This review covers risk assessment tools, pharmacologic prophylaxis selection, extended thromboprophylaxis after orthopedic surgery and cancer surgery, and the role of DOACs in medical prophylaxis.

Chronic Heart Failure Monitoring: NT-proBNP Guided Therapy
Natriuretic peptide-guided heart failure management remains debated despite multiple randomized trials. This review evaluates NT-proBNP targets, the GUIDE-IT trial limitations, and practical strategies for incorporating biomarker trends into therapeutic decision-making.

Anaphylaxis Management: Epinephrine Dosing and Biphasic Reactions
Epinephrine remains the only first-line treatment for anaphylaxis, yet it is delayed or withheld in up to 40% of cases. This review covers updated dosing guidelines, optimal route and site of administration, biphasic reaction risk factors, and observation period recommendations.

Cirrhosis Complications: Variceal Bleeding, Ascites, and Hepatic Encephalopathy Management
Decompensated cirrhosis demands systematic management of its life-threatening complications. This review covers current evidence for variceal hemorrhage prophylaxis and treatment, refractory ascites interventions, and hepatic encephalopathy targeting including rifaximin and lactulose protocols.

Urinary Tract Infections: Antimicrobial Selection and Resistance Patterns
UTI management is complicated by rising fluoroquinolone resistance and ESBL-producing E. coli prevalence. This review covers updated empiric therapy guidelines for uncomplicated cystitis, pyelonephritis, and complicated UTI, with resistance-informed prescribing strategies.
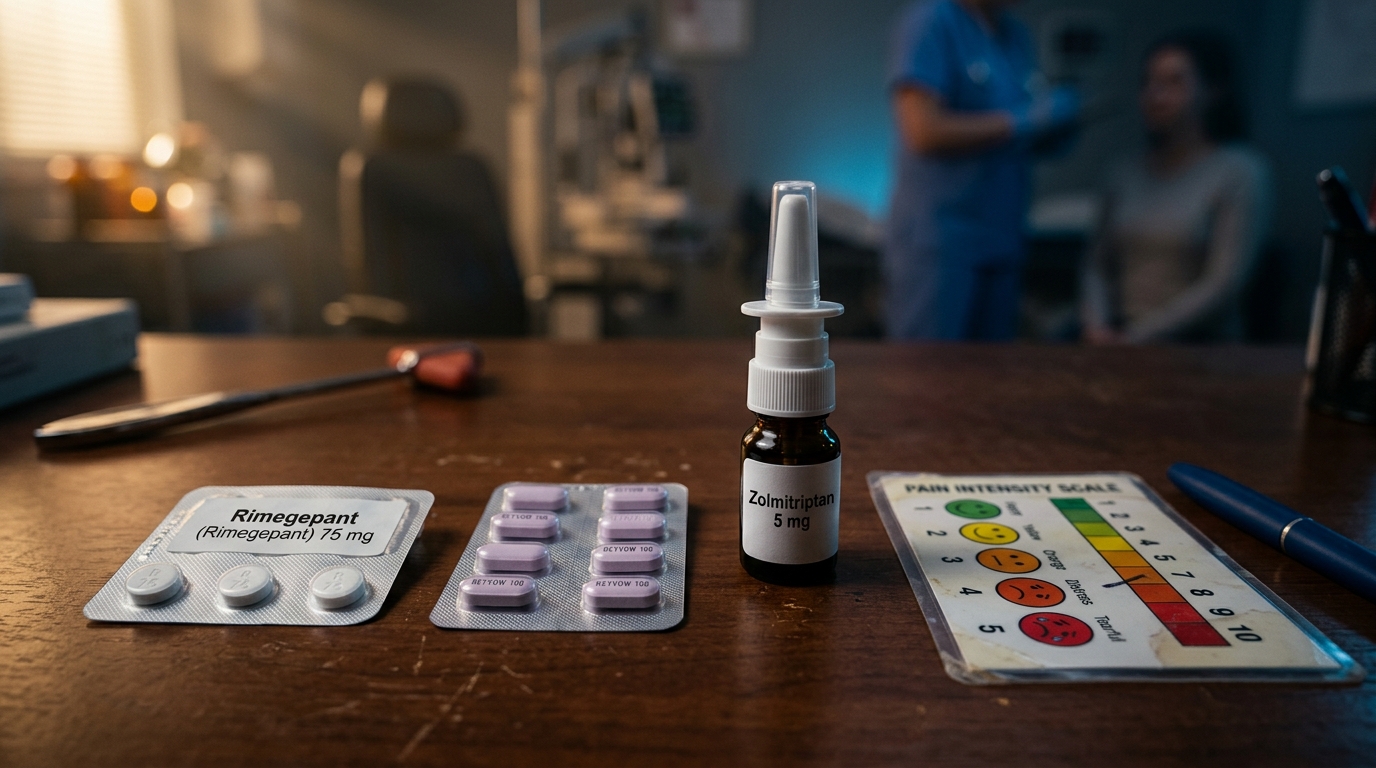
Migraine Acute Treatment: Gepants, Ditans, and Triptan Comparison
CGRP receptor antagonists (gepants) and 5-HT1F agonists (ditans) have expanded acute migraine pharmacotherapy beyond triptans for the first time in decades. This review compares efficacy, tolerability, and positioning of these drug classes with practical prescribing guidance.
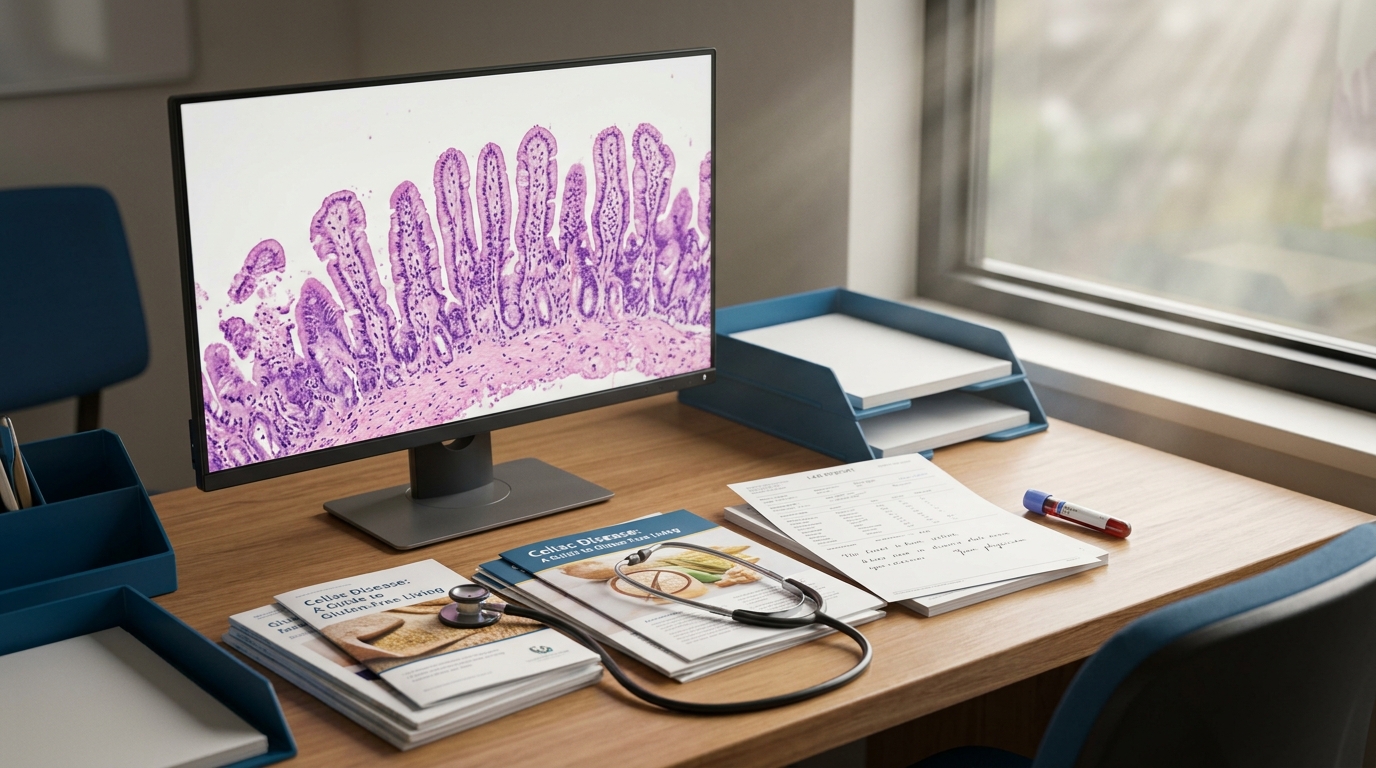
Celiac Disease Diagnosis: Serology, Biopsy, and Gluten-Free Management
Celiac disease affects approximately 1% of the population but remains underdiagnosed by a factor of 3-5. Current diagnostic algorithms combine tissue transglutaminase antibodies with duodenal biopsy, though emerging evidence supports serology-only diagnosis in select populations.
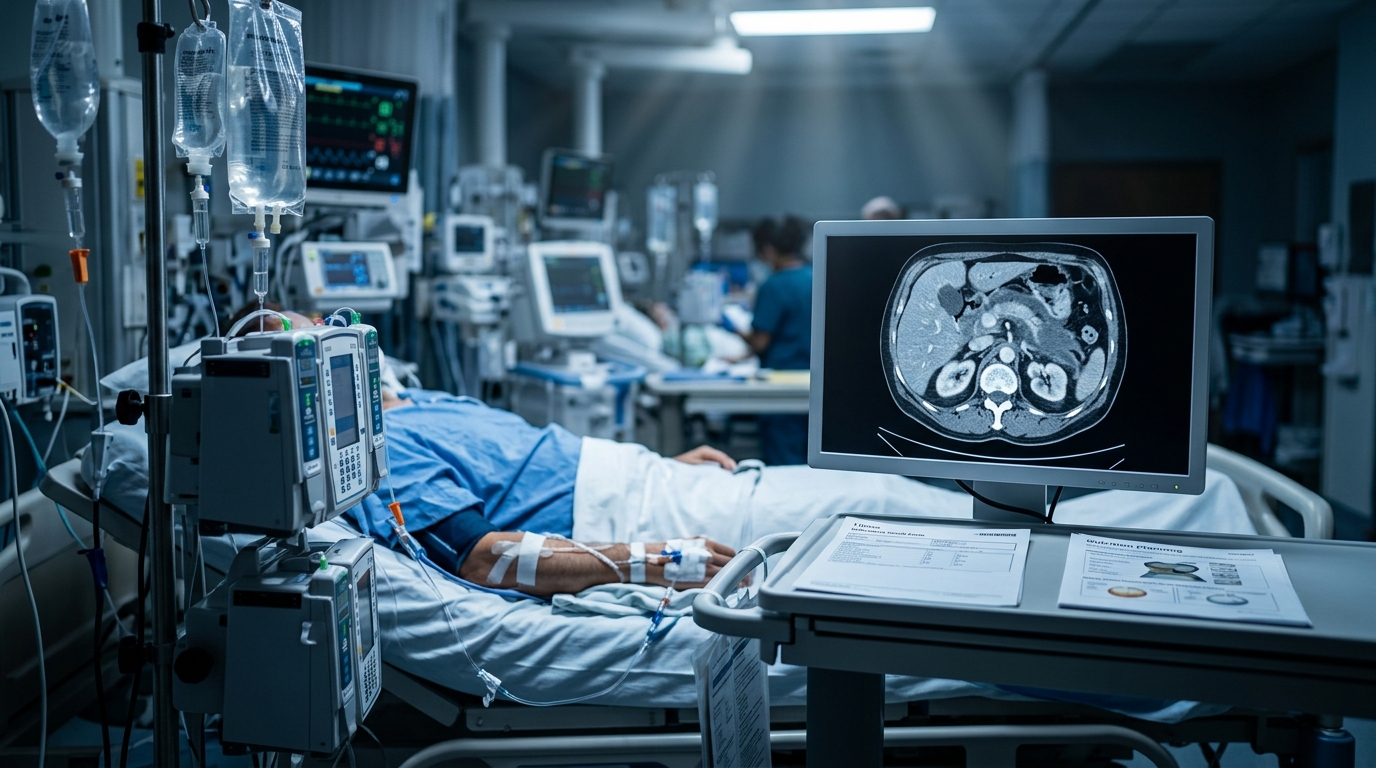
Acute Pancreatitis Management: Fluid Resuscitation and Nutrition Timing
Acute pancreatitis management has shifted significantly in the past five years, with goal-directed fluid resuscitation replacing aggressive hydration and early oral feeding supplanting prolonged fasting. This review covers the WATERFALL trial, nutrition strategies, and severity-stratified management.

ADHD in Adults: Diagnosis, Stimulant Selection, and Cardiovascular Monitoring
Adult ADHD affects 4-5% of adults and is increasingly diagnosed in primary care. This review covers validated diagnostic instruments, evidence-based pharmacotherapy selection between methylphenidate and amphetamine formulations, and cardiovascular safety monitoring requirements.
Endometriosis Management: Hormonal Therapy and Surgical Decision-Making
Endometriosis affects approximately 10% of reproductive-age women, with an average diagnostic delay of 7-10 years. This review covers empiric hormonal therapy, imaging advances, and evidence-based surgical approaches for pelvic pain and infertility.

Parkinson's Disease: Levodopa Optimization and Adjunctive Therapies
Motor fluctuations develop in approximately 50% of Parkinson's disease patients within 5 years of levodopa initiation. This review covers optimal levodopa dosing strategies, adjunctive therapy selection, and emerging device-based interventions for motor and non-motor symptoms.
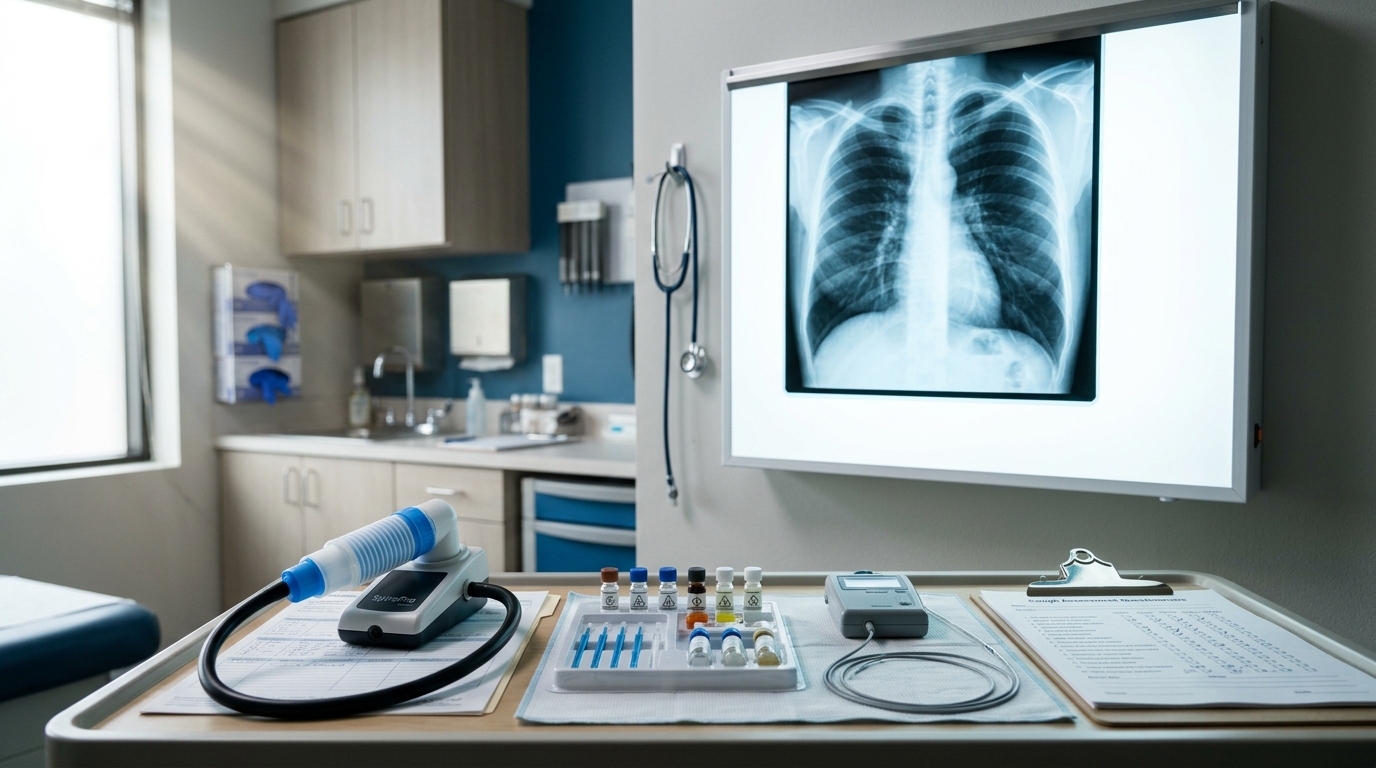
Chronic Cough Evaluation: A Systematic Diagnostic Approach
Chronic cough, defined as cough persisting beyond 8 weeks, affects 10-12% of the general population. A systematic algorithm targeting the three most common etiologies (upper airway cough syndrome, asthma, and GERD) resolves 85-95% of cases when applied rigorously.
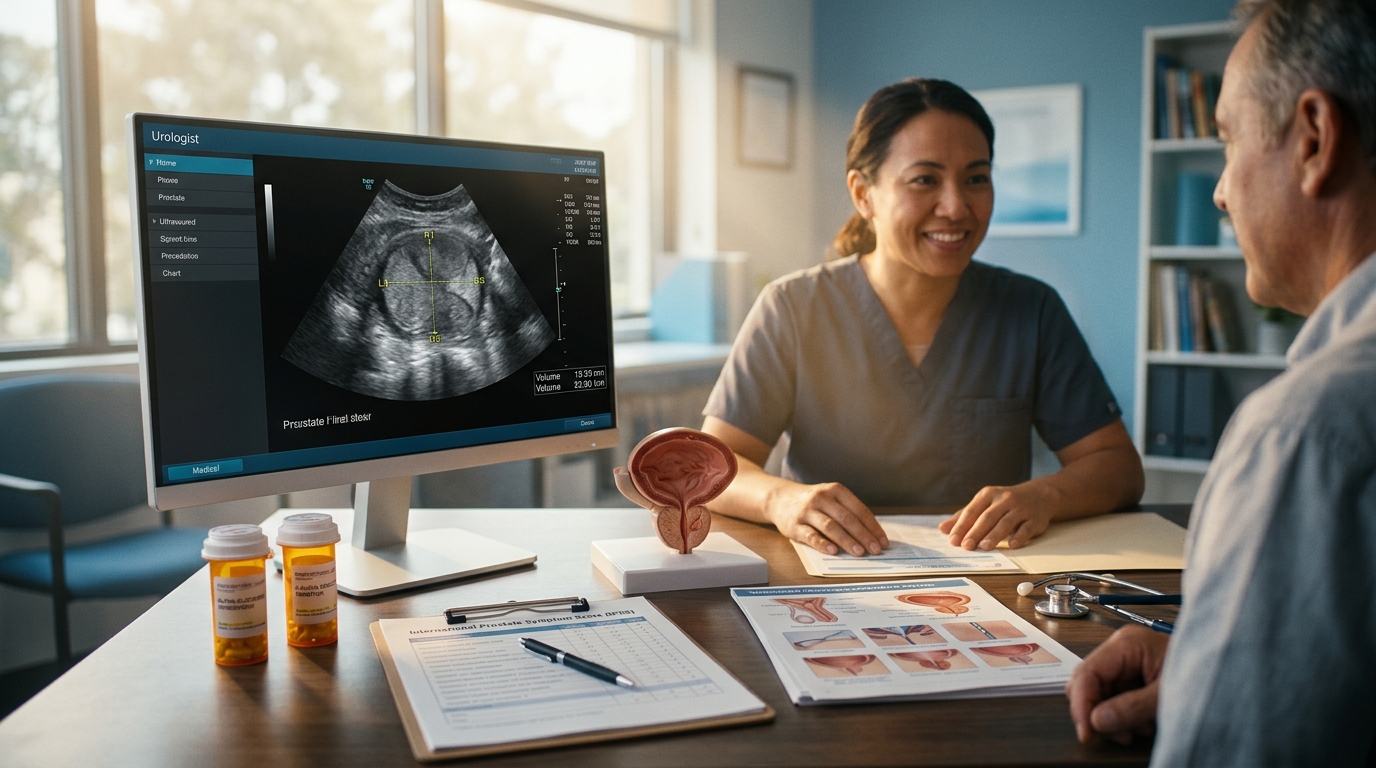
Benign Prostatic Hyperplasia: Medical Therapy Comparison and Surgical Options
BPH affects 50% of men by age 60 and 90% by age 85. Alpha-blockers, 5-alpha reductase inhibitors, and combination therapy provide effective medical management, while minimally invasive surgical therapies offer durable alternatives with favorable risk profiles.

Status Epilepticus: Updated Treatment Algorithm and Refractory Management
Status epilepticus carries a mortality rate of 10-30% and requires a time-critical, protocolized approach. The ESETT trial has standardized second-line therapy selection, while emerging evidence guides management of refractory and super-refractory cases.
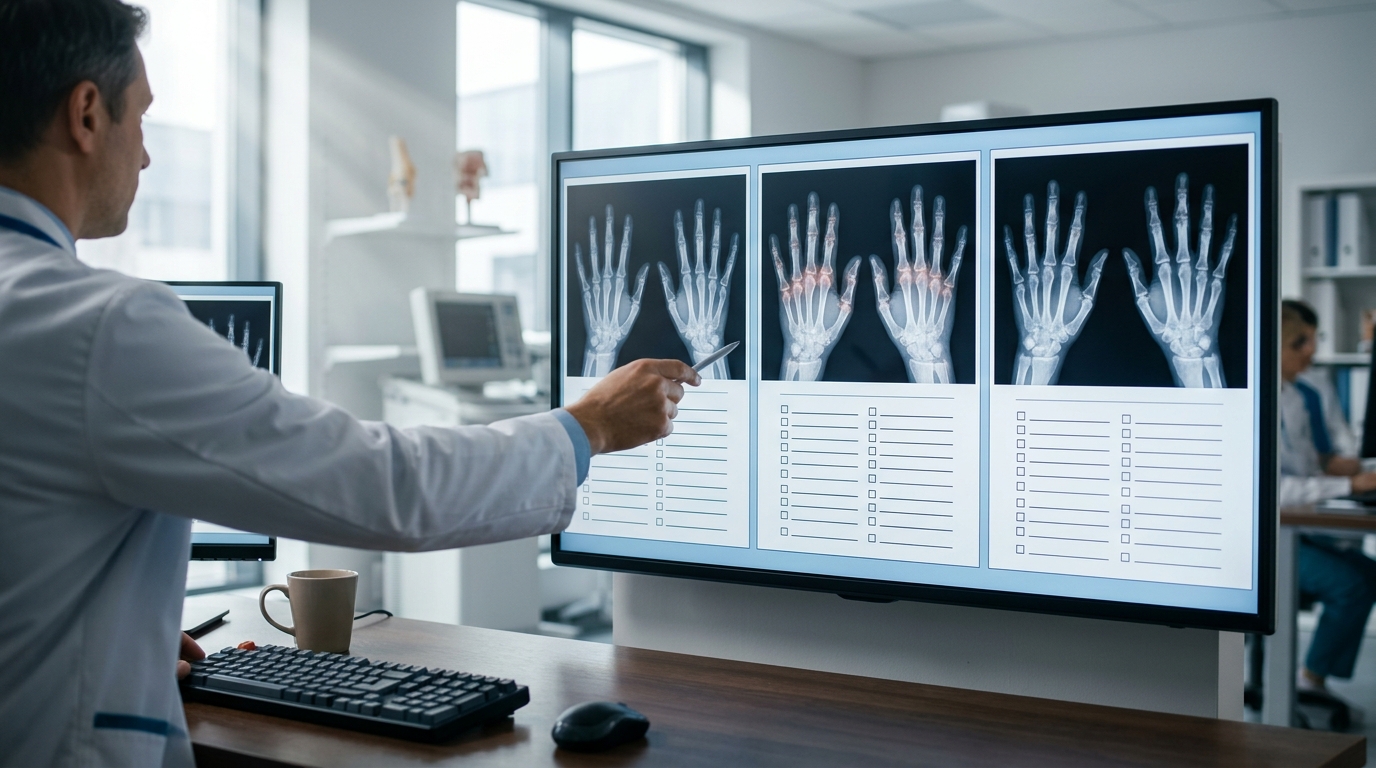
Inflammatory Arthritis Differential: RA vs PsA vs SpA Clinical Features
Distinguishing rheumatoid arthritis from psoriatic arthritis and spondyloarthritis is essential for targeted therapy selection. This review compares clinical patterns, serologic markers, imaging findings, and classification criteria across these three inflammatory arthritides.

Concussion Management: Return-to-Play Protocols and Persistent Symptoms
Sport-related concussion management has evolved significantly with the 2023 Amsterdam Consensus Statement. Current protocols emphasize individualized recovery timelines, graduated return-to-play progression, and evidence-based management of persistent post-concussion symptoms.

Polypharmacy in Elderly Patients: An Evidence-Based Deprescribing Framework
Your 82-year-old patient takes twelve medications. Each one was individually appropriate when prescribed. The problem is not any single drug — it is the cumulative burden of all of them in an aging body. Here is a structured approach to deciding what to stop, and in what order.

Interpreting Elevated hs-CRP in the Context of Multiple Comorbidities
Your 64-year-old patient has an hs-CRP of 8.2 and carries five diagnoses that all cause inflammation. The CRP is elevated. By which condition? All of them? Or something new you have not found yet?

Tools for Complex Multi-System Cases: What Physicians Need
Complex multi-system cases challenge traditional clinical tools because the answer lives at the intersection of specialties. Here is why these cases are hard, what an ideal tool would do, and what the evidence shows.
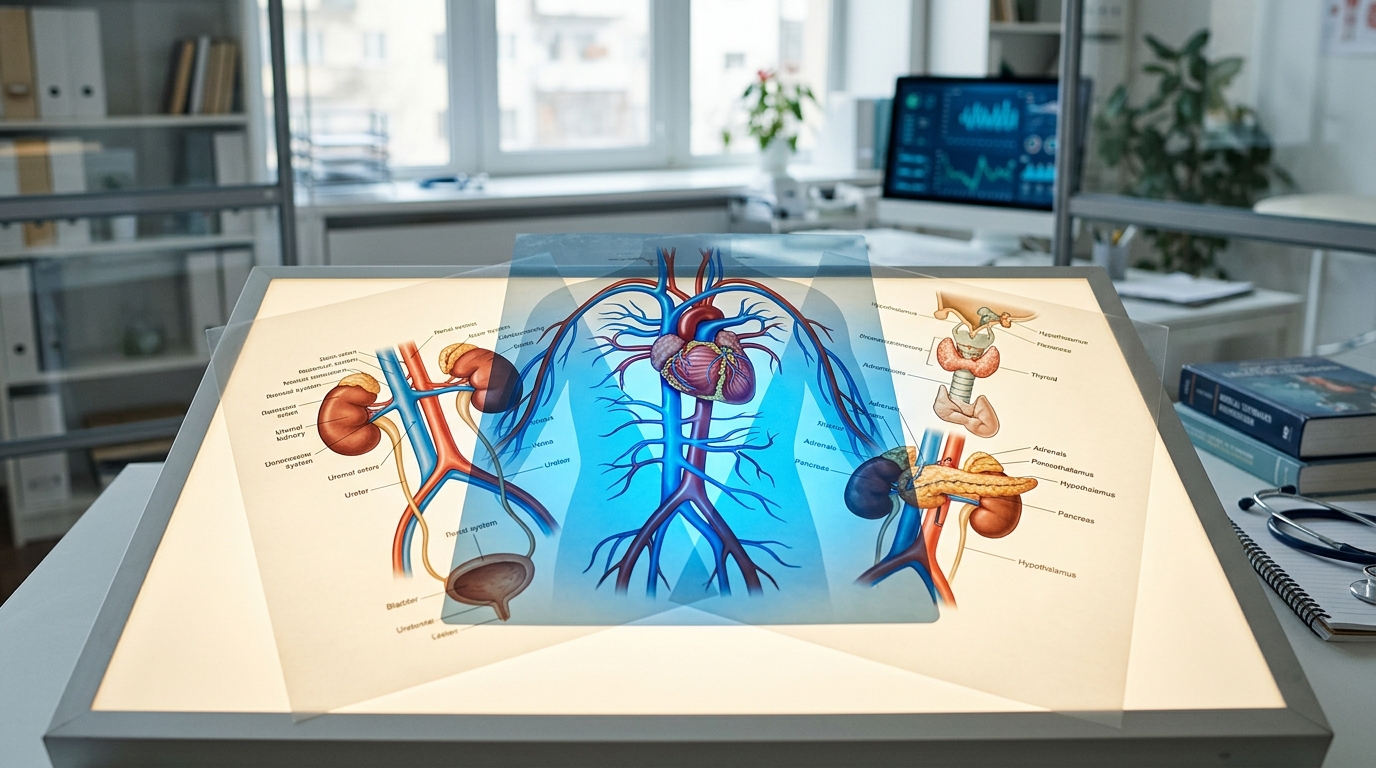
Cross-System Clinical Reasoning: Why No Single Specialty Has the Full Picture
Cross-system clinical reasoning connects evidence across organ systems and specialties to reveal diagnoses and treatment strategies that no single specialty perspective would identify. Here is why it matters, with detailed case examples.
When Depression Doesn't Respond to SSRIs: A Cross-System Differential
Before you add an atypical antipsychotic to that SSRI, check the thyroid, the B12, the CRP, and the sleep study. A structured cross-system evaluation reveals treatable causes in up to 40% of cases labeled treatment-resistant.
Showing 1–28 of 28 articles