Migraine Acute Treatment: Gepants, Ditans, and Triptan Comparison
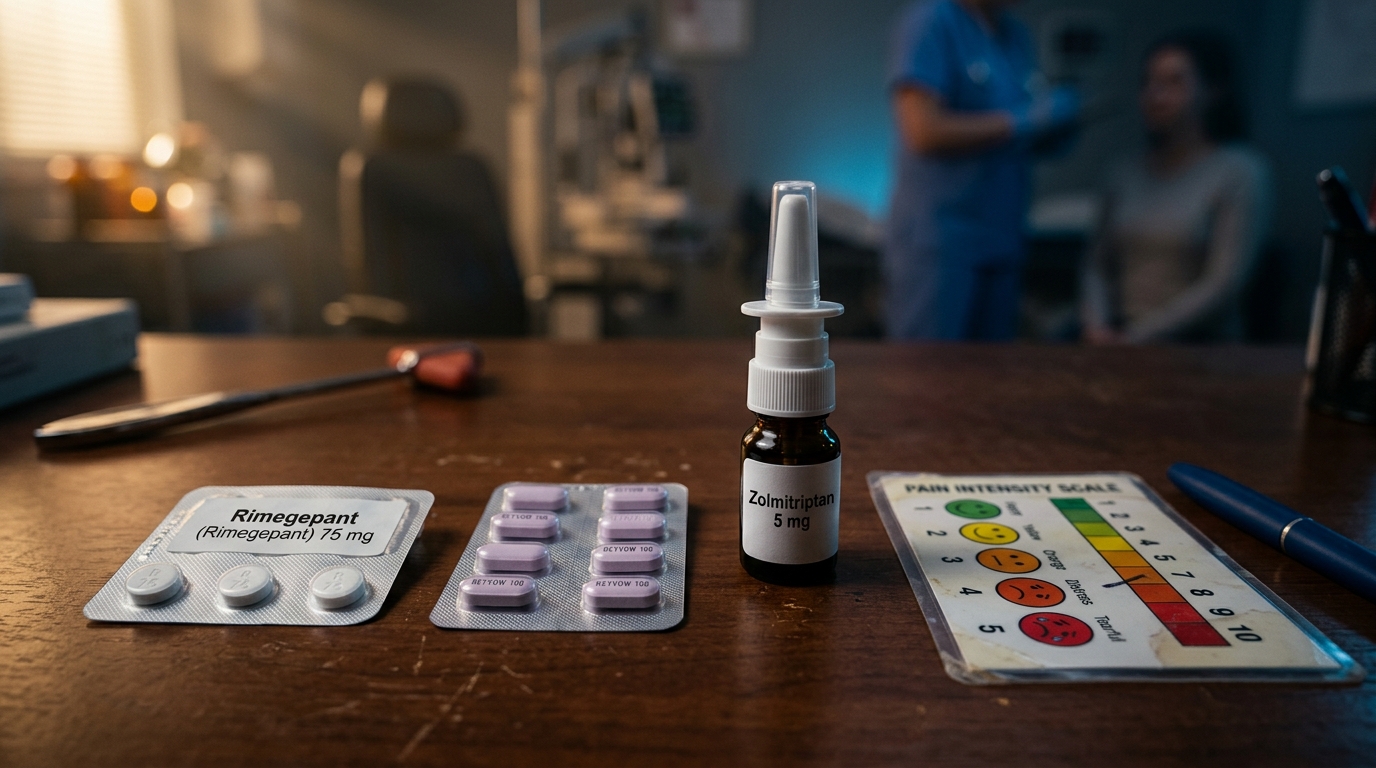
Triptans: The Established Standard
For the neurologist, headache specialist, or primary care physician managing migraine patients, the acute treatment landscape has expanded beyond triptans for the first time in decades. Gepants and ditans offer mechanism-specific alternatives that address the large population of patients with cardiovascular contraindications to triptans or insufficient triptan response. Understanding how these drug classes compare — in efficacy, safety, onset, and practical prescribing — is now essential for making individualized acute migraine treatment decisions.
Triptans (5-HT1B/1D agonists) remain the most effective acute migraine treatment class for most patients. Sumatriptan 100 mg oral achieves pain freedom at 2 hours in approximately 30-35% of patients, with rizatriptan 10 mg and eletriptan 40 mg showing modestly higher 2-hour pain-free rates of 35-40%[1] in network meta-analyses. Triptans are contraindicated in patients with established cardiovascular disease, uncontrolled hypertension, hemiplegic migraine, or basilar migraine due to their vasoconstrictive properties. Approximately 30-40% of migraine patients have contraindications to or insufficient response to triptans[1], creating a significant unmet need that gepants and ditans now address.
Gepants: CGRP Receptor Antagonists
Two oral gepants are approved for acute migraine treatment: ubrogepant (50 mg and 100 mg) and rimegepant (75 mg ODT). In the ACHIEVE I trial, ubrogepant 100 mg achieved 2-hour pain freedom in 21.2% versus 11.8% placebo (p < 0.001) and 2-hour most bothersome symptom (MBS) freedom in 37.7% versus 27.8%[1]. Rimegepant 75 mg achieved 2-hour pain freedom in 19.6% versus 12.0% placebo[2]. While these pain-free rates are numerically lower than triptans, gepants offer critical advantages: no vasoconstrictive properties (safe in cardiovascular disease), no risk of medication overuse headache (MOH), and rimegepant has dual approval for both acute treatment and preventive use (every other day dosing). The most common adverse effects are nausea (2-4%) and somnolence (1-2%), with no triptan-like chest tightness or paresthesias.
Lasmiditan: The First Ditan
Lasmiditan (Reyvow), a selective 5-HT1F agonist, activates serotonin receptors involved in trigeminal pain signaling without vasoconstrictive 5-HT1B effects. The SAMURAI and SPARTAN trials demonstrated 2-hour pain freedom rates of 28-32% for lasmiditan 200 mg versus 15-16% placebo[3]. The primary limitation is CNS side effects: dizziness (15-17%), somnolence (5-6%), and paresthesias (5-7%), with an 8-hour driving restriction after dosing[3]. Lasmiditan is classified as a Schedule V controlled substance due to its subjective effects profile, though abuse potential appears low. It is best positioned for patients with cardiovascular contraindications to triptans who tolerate CNS effects and do not need to drive after treatment.
Head-to-Head Data and Positioning
Direct comparison data remain limited. The Phase 4 COURAGE trial is evaluating ubrogepant versus eletriptan head-to-head. Indirect treatment comparisons and network meta-analyses consistently rank triptans (particularly eletriptan, rizatriptan, and sumatriptan) as having the highest acute efficacy, followed by lasmiditan, then gepants. However, efficacy is only one dimension: consistency of response, tolerability, safety profile, and patient-reported satisfaction must all inform selection. Patients with cardiovascular disease or multiple vascular risk factors should receive gepants or lasmiditan. Patients prioritizing avoiding MOH may benefit from gepants. Patients with infrequent, severe attacks and no vascular contraindications may prefer triptans for maximal acute efficacy.
Combination and Multi-Mechanism Approaches
Combining a triptan with an NSAID (sumatriptan 85 mg/naproxen 500 mg, available as Treximet) achieves 2-hour pain-free rates of approximately 35-40%, superior to either agent alone. Emerging practice includes combining a gepant with a triptan for refractory attacks, though formal trial data for this combination are limited. Patients should treat early (within 1 hour of onset) for maximal efficacy across all drug classes. For patients with medication overuse headache (using acute treatments 10-15 or more days per month), transitioning to gepant-based acute therapy combined with preventive therapy (CGRP monoclonal antibody, gepant prophylaxis, or neuromodulation) is the recommended approach to break the MOH cycle.
A Practical Selection Framework for the Clinic
When a patient presents asking for an acute migraine treatment, the selection decision follows a clear logic. First, assess for cardiovascular contraindications. If none are present and the patient has infrequent, moderate-to-severe attacks, a triptan remains the best first choice — eletriptan or rizatriptan for patients wanting the highest acute efficacy, sumatriptan for the broadest formulation options (oral, nasal, injectable). If cardiovascular contraindications exist or the patient has failed triptans, gepants are the next step — ubrogepant for pure acute use, rimegepant if the patient also needs preventive coverage. Lasmiditan fills a narrow niche: the patient with cardiovascular disease who has failed gepants or needs stronger acute relief and can accept the driving restriction and CNS side effects. For every patient, early treatment within the first hour of attack onset is the single most impactful prescribing instruction, regardless of which drug class is chosen.
Limitations and What the Data Cannot Tell Us
The acute migraine treatment landscape suffers from a lack of large head-to-head trials between the newer agents and triptans. The efficacy rankings described here are derived primarily from indirect treatment comparisons and network meta-analyses — methods that are informative but not equivalent to direct randomized comparisons. Individual patient response to migraine treatments is notoriously variable: a patient who does not respond to one triptan may respond dramatically to another, and the same unpredictability applies to gepants. Cost and insurance coverage remain significant barriers to accessing newer agents, with many patients unable to obtain gepants or lasmiditan without substantial out-of-pocket expense. The most practical advice for the treating clinician is to have familiarity with all three drug classes and to match the selection to the individual patient's cardiovascular profile, attack characteristics, lifestyle constraints, and treatment history.
References
- Ubrogepant for the Treatment of Migraine (ACHIEVE I, Dodick et al., JAMA 2019) PubMed 31291514
- Efficacy, Safety, and Tolerability of Rimegepant 75 mg for the Acute Treatment of Migraine (Croop et al., Lancet 2019) PubMed 31311674
- Lasmiditan for Acute Treatment of Migraine (SPARTAN/SAMURAI, Goadsby et al., 2019) PubMed 31132795
Frequently Asked Questions
What is the 2-hour pain freedom rate for ubrogepant vs triptans?
Are gepants safe in patients with cardiovascular disease?
Does lasmiditan have driving restrictions after dosing?
Which acute migraine treatment avoids medication overuse headache?
When should I consider combining a triptan with an NSAID?
What is the NNT for lasmiditan vs placebo in acute migraine?
Explore This Topic in Ailva
Ailva is a free clinical intelligence platform for NPI-verified US physicians. Get evidence-based answers with verified citations from 16M+ indexed papers — plus free CME credits.

Founder of Ailva.ai | Former Director of Research and Author of 200+ Medically Reviewed Articles | Editor-in-Chief of EudaLife Magazine